Chorionic villus sampling (CVS), or chorionic villus biopsy, is a prenatal test that involves taking a sample of tissue from the placenta to test for chromosomal abnormalities and certain other genetic problems. The placenta is a structure in the uterus that provides blood and nutrients from the mother to the fetus.
The chorionic villi are tiny projections of placental tissue that look like fingers and contain the same genetic material as the fetus. It is these villi which are used for genetic testing
Chorionic villus sampling may be used for genetic and chromosome testing in the first trimester of pregnancy. Here are some reasons that a woman might elect to undergo CVS:
There may be other reasons for your doctor to recommend a chorionic villus sampling.
Getting the test done is completely your choice. We can suggest what is good practice based on evidence-based medicine. Knowing all the pros and cons, you can accept or decline the testing.
CVS is usually done between 11-12 weeks of pregnancy.
The fetal medicine specialist will explain the procedure to you and offer you the opportunity to ask any questions that you might have about the procedure. You will be asked to sign few consent forms that gives the permission to do the procedure. There is no special restriction on diet or activity prior to chorionic villus sampling.
Your doctor will note if you are allergic to any medications, latex, iodine, tape, and anesthetic agents (local and general), medications that you are taking, any history of bleeding disorders or any anticoagulant (blood-thinning) medications, aspirin, or any other medications that may affect blood clotting. It may be necessary for you to stop these medications prior to the procedure. Your blood group will also be noted and if you are Rh negative, an injection anti-D will be given to you after the procedure.
An ultrasound will be performed to check the fetal heart rate and the position of the placenta and the fetus. The fetus is also assessed for structural abnormality. CVS can be done abdominally and transcervically.
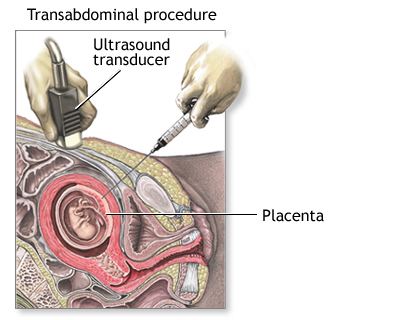
We generally do it transabdominally. A local anesthetic is injected into the skin. You will feel a needle stick when the anesthetic is injected. This may cause a brief stinging sensation. Then, ultrasound will be used to help guide a long, thin, hollow needle through your abdomen and into the uterus and placenta. This may be slightly painful, and you may feel a cramp as the needle enters the uterus. Tissue will be gently suctioned into a syringe. More than one sample may be needed to obtain enough tissue for testing. The needle will then be removed. An adhesive bandage will be placed over the abdominal needle insertion site.
You are made to rest for half an hour after the procedure. The fetal heart beat is checked and then you are sent home. Most women have no problems, but you might have a bruise, spotting or cramping. If you do, paracetamol is safe to take. If you have a persistent pain, leaking, bleeding or a high temperature, then you need to go to the hospital.
There is minimal risk of miscarriage about 3: 1000. It does not cause any birth defects or any harm to the mother. The risk of infection is also very low, 1 in 1000.
You can consult with Dr. Neha Gupta. She is one of the best fetal medicine specialists and is experienced in handling lots of pregnant women to take care of their unborn baby. Contact us to get the appointment and discuss it with her.